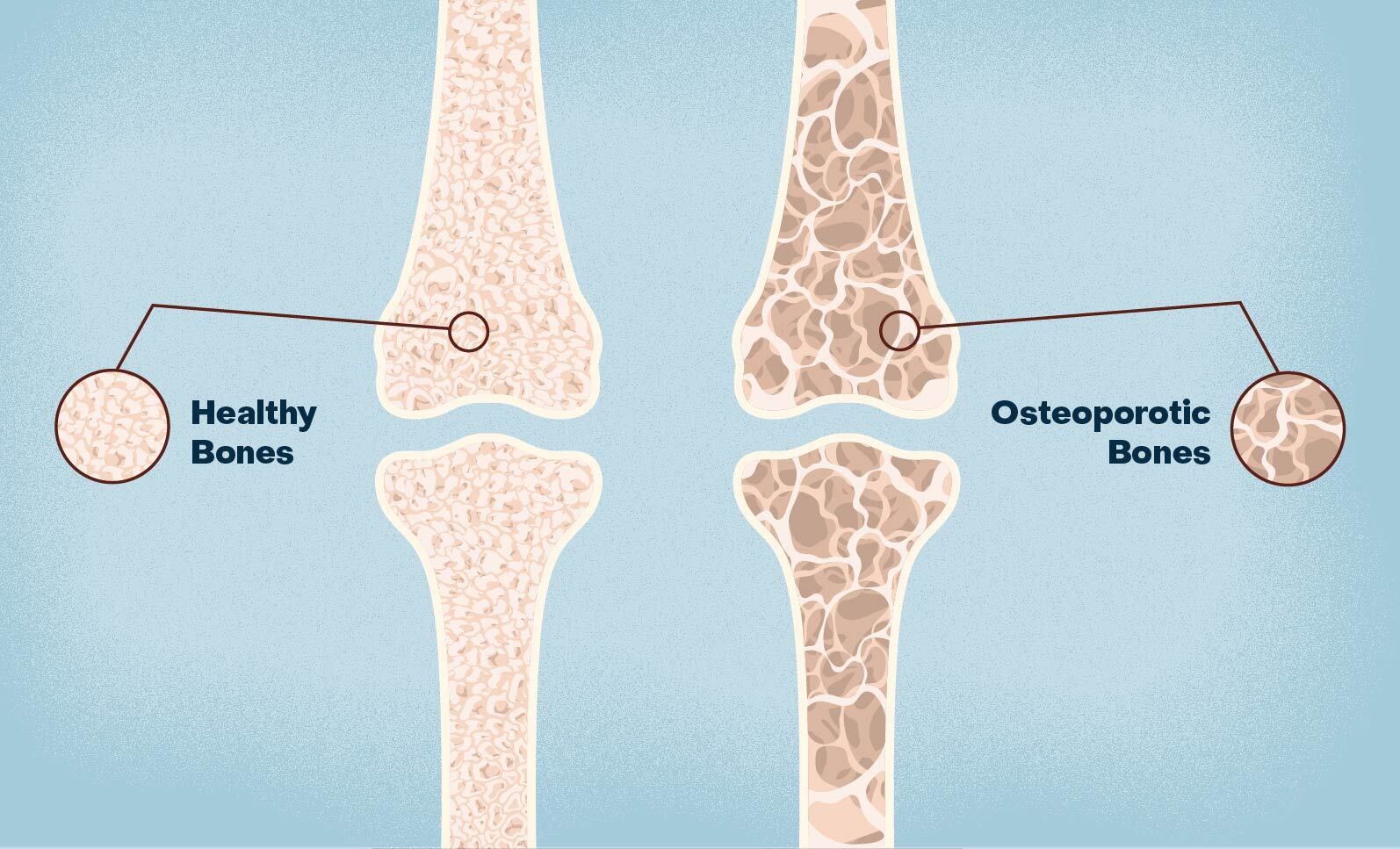
Osteoporosis is a disease characterized by low bone mass and microarchitectural deterioration, leading to increased bone fragility and susceptibility to fractures. There are some factors that contribute to this such as inadequate peak bone mass, excessive bone resorption and adequate formation of new bone during the remodeling stage. Typically, as we age, there will be some changes in our hormones that will slow down the rate of our bone formation while the rate of bone resorption keeps increasing. This is a normal process of the human body when aging which we can’t control. This condition is particularly prevalent among older adults and postmenopausal women. A lot of recent studies shows that even if we can’t stop or reverse this condition, we can actually control the rate of bone loss by doing physical activity.
Physical activity and exercises have been recognized as effective measures for reducing the risk of osteoporosis and improving bone density. According to DJ Wilson (2019), “physical activity is an important factor in the development and maintenance of bone health, and regular exercise can reduce the risk of osteoporotic fractures”.
For people with osteoporosis specifically, it is recommended a combination of resistance and endurance training prioritizing for exercises that involves weight bearing according to the patient exercise capacity because it will help to increase the muscle strength and therefore reduce stress on the bones when moving. As studies has shown that muscle strength has a positive association with bone health (Torres-Costoso et al., 2020) Physical activities can also help with improving balance and reduce the risk of falls, which is a significant concern not just for osteoporosis patient but also for older adults.
Understanding the Role of Exercise in Osteoporosis: A Balanced Approach
Before beginning any treatment, it’s crucial for patients to understand the risks involved, especially when dealing with osteoporosis. While it’s true that certain physical activities and high-impact movements can increase the risk of fractures, exercise isn’t the enemy. In fact, it’s one of the most powerful tools we have to manage and potentially reduce that risk.
Research shows that physical activity is a modifiable risk factor for osteoporotic fractures (Moayyeri, 2008). This means that, with the right approach, we can turn movement into medicine. The key lies in finding the right type, intensity, and duration of exercise that supports bone health without causing harm.
That’s why personalized exercise programs are so important. They should be tailored to each individual’s age, fitness level, and medical history. There’s no universal solution when it comes to exercise and osteoporosis. And as our bodies change over time, so should our exercise routines. Ongoing monitoring and reassessment ensure that these programs stay safe and effective (Beck et al., 2017).

Exercise Recommendations
The American College of Sports Medicine (ACSM) suggested that people with osteoporosis should do activities such as :
- Walking, dancing or stair climbing for at least 30 minutes per day, most days of the week.
- Resistance exercises such as weight lifting or using resistance bands should be performed for 2 to 3 times per week with 1 to 3 sets of 8 to 12 repetitions per exercise.
- Balance exercises such as standing on one leg or walking heel to toe should be performed daily to reduce risk of falls. For the intensity, patients should aim to exercise at moderate intensity which is equivalent to a 5 to 6 scale of 0 to 10 rate of exertion (RPE) scale, where 0 represent no exertion and 10 is maximal exertion.
However, the intensity of the exercise should be individualized based on the patient fitness level and medical history. The duration and intensity should be gradually increasing over time while monitoring the symptoms and adjusting their program as needed. It is recommended for the patient to exercise under the supervision of qualified therapist (Physiotherapist/ Exerise Physiologist / Clincal Exercise Physiologist ) to ensure their safety.

Potential Barriers and How to Overcome it
For many individuals living with osteoporosis, the idea of starting an exercise program can feel overwhelming. Pain, discomfort, and limited mobility are common barriers that make physical activity seem out of reach. However, managing chronic pain doesn’t rely solely on medication. While pain relief drugs play a role, non-pharmacological approaches such as targeted physical activity can significantly improve mobility, strengthen muscles, and reduce stress on the bones, ultimately helping to ease pain (Paolucci et al., 2016).
Mental health challenges, such as anxiety and depression, are also common among osteoporosis patients. These emotional barriers can be just as limiting as physical ones. Interestingly, a study by Zhang (2017) highlighted how rehabilitation programs based on the Health Belief Model (HBM) can make a real difference. This approach encourages patients to reflect on their personal risk of further injury and weigh the benefits of exercise against perceived obstacles—like discomfort, lack of motivation, or fear of making things worse. For clearer picture of the HBM, see below for more info:
By addressing both the physical and psychological hurdles, we can create a more compassionate and effective pathway to recovery—not through a one-size-fits-all method, but with personalized strategies that empower each patient to move forward at their own pace.

To summarize, physical activity is important for people with osteoporosis as it slows down the rate of your bone loss while strengthening your muscles to support your bone and joint health. It is recommended to get proper assessment before planning on doing any activities. Other than that, it is better to get advice from a certified doctor, physiotherapist or clinical exercise physiologist to get a proper exercise prescription like what kind of exercise or activities that suites the patient current level. Physical activity and exercise can still be considered as a risk if it is not done with the suitable intensity and under proper supervision. If you have a family member with the condition, always encourage them to do more physical activities as it’s proven that they are beneficial while giving constant positive reinforcement to help with their anxiety and lack of confidence to engage with the exercise program and reduce the risk of fractures.

Refferences
Beck, B. R., Daly, R. M., Singh, M. a. F., & Taaffe, D. R. (2017). Exercise and Sports Science Australia (ESSA) position statement on exercise prescription for the prevention and management of osteoporosis. Journal of Science and Medicine in Sport, 20(5), 438–445. https://doi.org/10.1016/j.jsams.2016.10.001
Moayyeri, A. (2008). The Association Between Physical Activity and Osteoporotic Fractures: A Review of the Evidence and Implications for Future Research. Annals of Epidemiology, 18(11), 827–835. https://doi.org/10.1016/j.annepidem.2008.08.007
Torres-Costoso, A., López-Muñoz, P., Martínez-Vizcaíno, V., Álvarez-Bueno, C., & Cavero-Redondo, I. (2020). Association Between Muscular Strength and Bone Health from Children to Young Adults: A Systematic Review and Meta-analysis. Sports Medicine, 50(6), 1163–1190. https://doi.org/10.1007/s40279-020-01267-y
Wilson, D. (2019). Osteoporosis and sport. European Journal of Radiology, 110, 169–174. https://doi.org/10.1016/j.ejrad.2018.11.010
Zhang, M. (2017). Effect of HBM Rehabilitation Exercises on Depression, Anxiety and Health Belief in Elderly Patients with Osteoporotic Fracture. Psychiatria Danubina, 29(4), 466–472. https://doi.org/10.24869/psyd.2017.466
Prepared by
Putera Irfan
Your Physio Ampang

